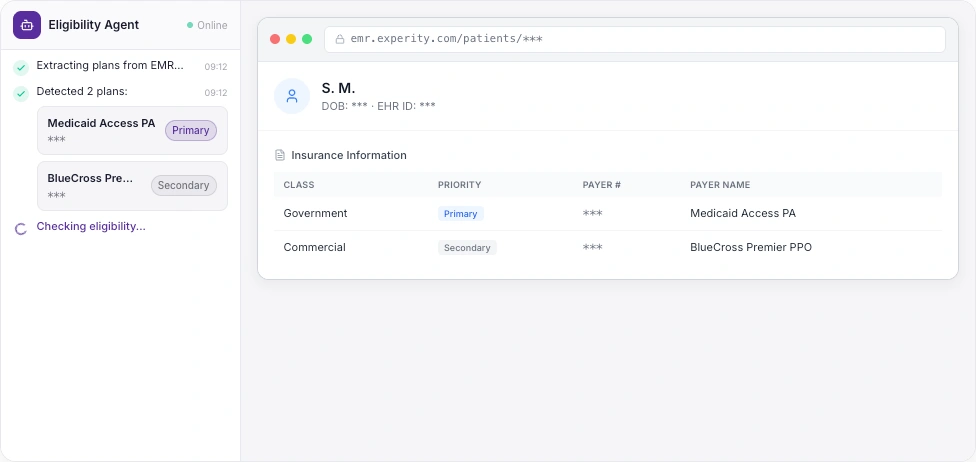
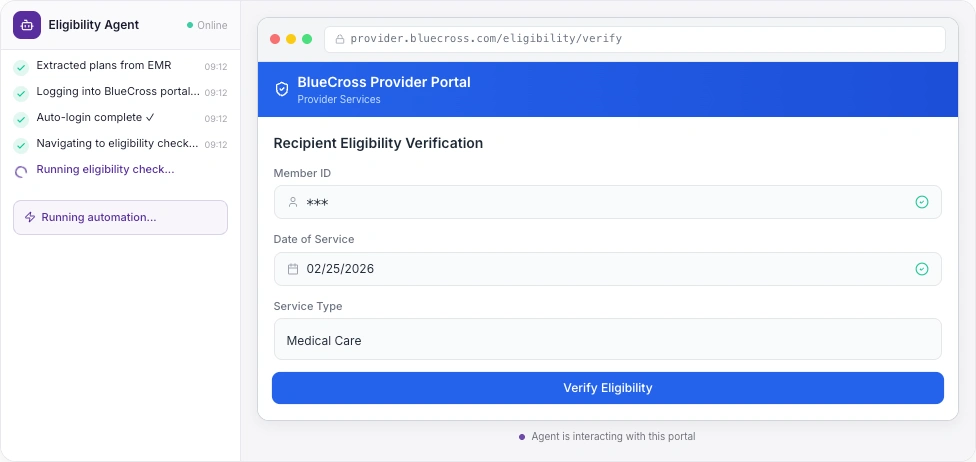
Your Front Desk Has More Important Things to Do
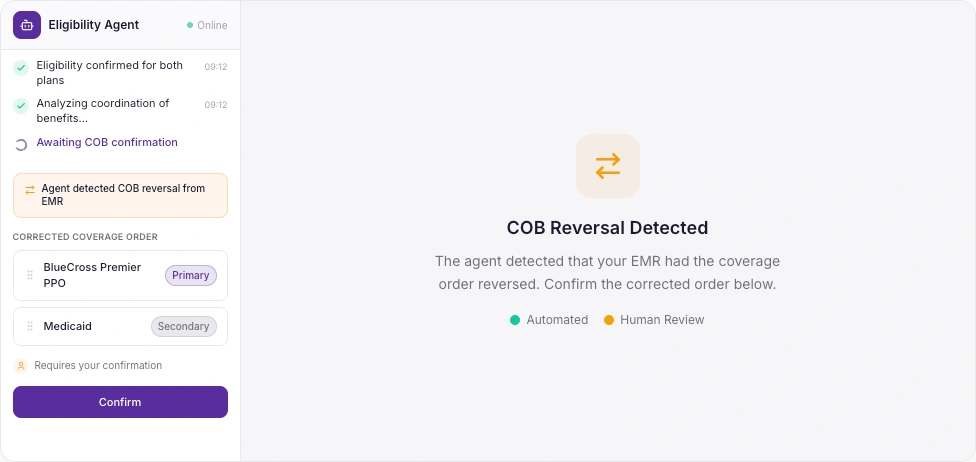
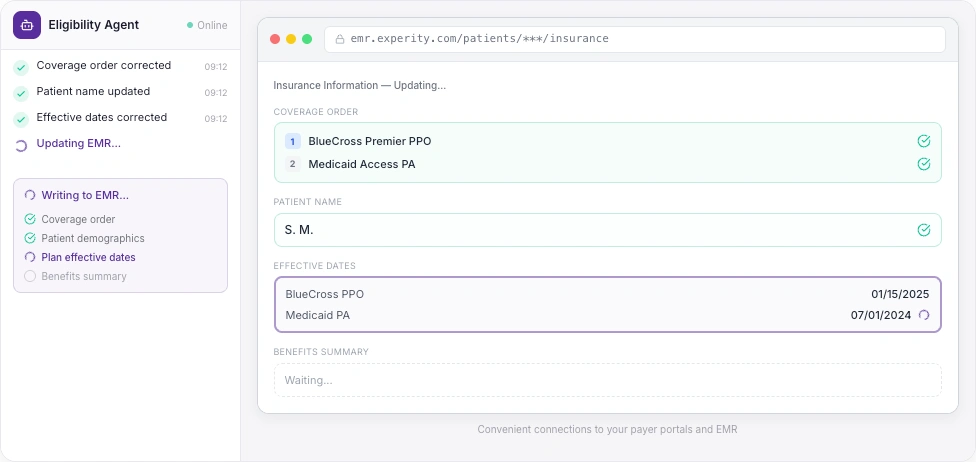
💬Below is the COB order as per your EMR. Confirm or reorder.
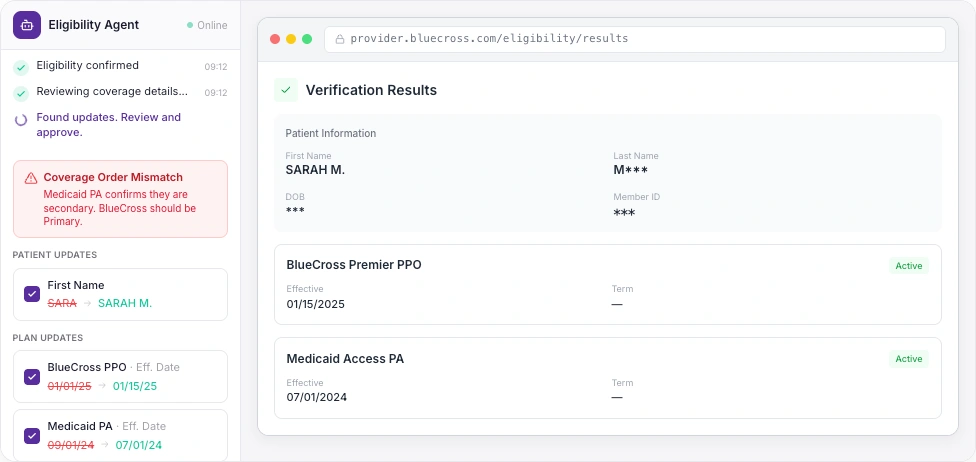
💬I found updates to post to your EMR. Review and click Update.
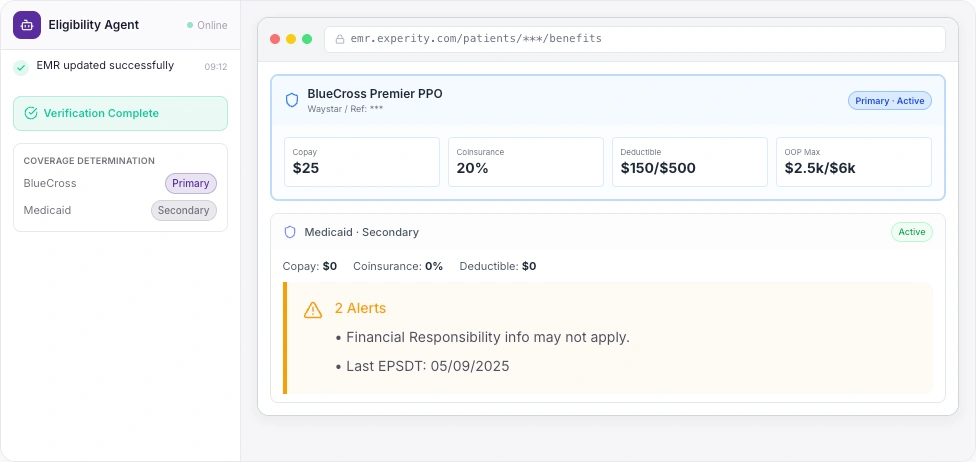
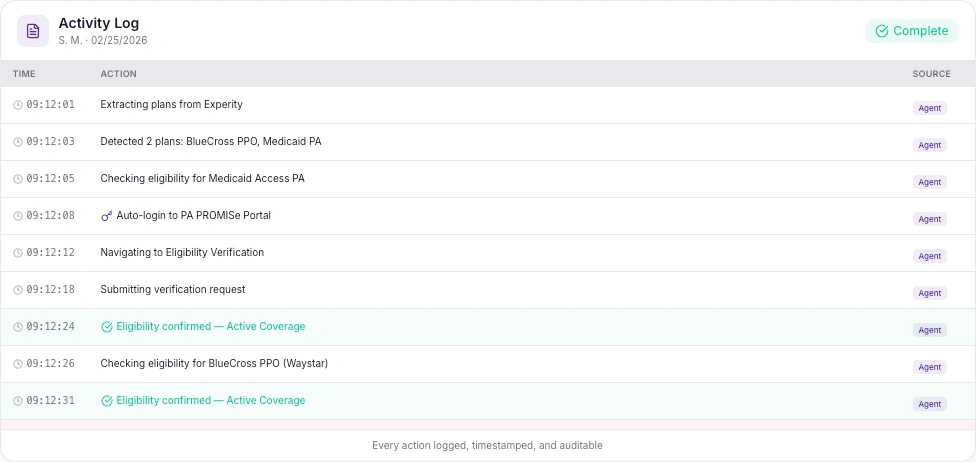
Every action visible. Every step auditable.
The Eligibility Process Is Broken - And You Only Find Out When It's Too Late
Portal Chaos
Front desk staff must log into dozens of payer portals, each with different interfaces, credentials, and data formats. There's no way to track if they're actually doing it.
Data Entry Errors
Even when staff check the portal correctly, manually re-entering coverage details into the EMR introduces errors that travel downstream to claims.
Knowledge Walks Out the Door
Front desk has the highest attrition in any practice. Every departure takes portal knowledge, login credentials, and workflow understanding with it.
One Click. Full Verification. Zero Data Entry.
Built for How Your Practice Actually Works
Mitigate Risk
Every skipped or botched eligibility check is money lost downstream. The Eligibility Agent creates an auditable record that every patient's coverage was verified before treatment - protecting your revenue at the source.
Reduce Turnover Pain
Front desk staff have the highest attrition in healthcare practices. The Eligibility Agent eliminates the need for portal-specific training, so new hires can be productive from day one. No more knowledge walking out the door.
Retain Your Best People
Nobody took a front desk job to fight with payer portals. By automating the most frustrating part of their workflow, the Eligibility Agent makes the job about what it should be - greeting patients and delivering great care experiences. Happier staff stay longer.